For weeks on end before your period arrives, a troublesome visitor shows up that many women would rather not see; painful and annoying new pimples. This is a symptom we’ve all come to call premenstrual acne and it’s pretty much a standard symptom of hormonal acne. It makes sense that acne tends to get worse just before your period for so many people.
It can really get under your skin – the frustration that is – especially when you’re already dealing with all the other annoying symptoms that come with being premenstrual. Your skin just seems to decide to get in on the action and start breaking out.
This article explains the biological rhythm behind premenstrual acne. Instead of offering a one-size-fits-all “fix,” we’ll explore the why—the hormonal shifts that drive breakouts, why standard advice sometimes misses the mark, and how a deeper understanding of your cycle can inform more supportive skincare choices.
Hormonal breakouts often appear around the chin and jawline — learn more in Chin Pimples: Why They Hurt and How to Care for Them.
The Monthly Pattern: Why Acne Flares Before Your Period
The classic monthly pattern is acne getting worse right before a period. Premenstrual acne is no random event though – there’s actually a pretty predictable timeline to it all. Typically this flare-up occurs in the luteal phase – that’s the one to two weeks that fall after ovulation and before your period kicks in.
For some people, the breakouts can start as early as 10 to 14 days before your period is due to arrive; others see them peak just before things start to flow. The acne tends to show up on the lower third of your face – think chin, jawline, and around the mouth, though it can pop up on the cheeks, neck, back, & shoulders too.
What sets premenstrual acne apart from other breakouts is its hormonal trigger. Now you might think that hormones are involved in all acne, and you’d be right. But premenstrual acne is different in that it’s directly linked to the natural ups and downs of sex hormones over the course of your menstrual cycle.
The Hormonal Timeline: What Happens in Your Cycle
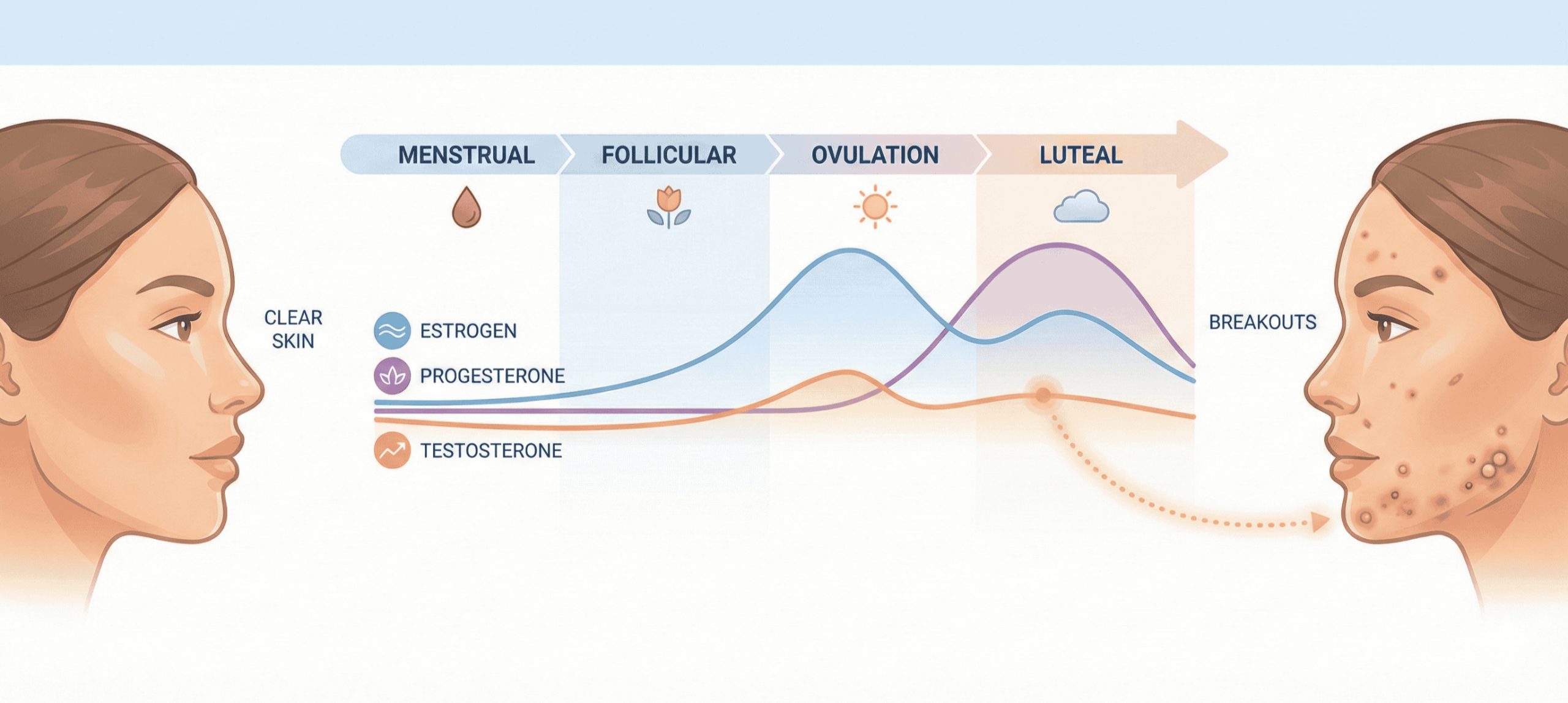
To understand the predictable pattern of premenstrual acne, it is essential to map its occurrence onto the specific hormonal fluctuations that define the menstrual cycle. The breakout you see on the skin’s surface is a direct physiological response to the sequenced rise and fall of key reproductive hormones beneath the surface.
The Luteal Phase: The Core “Pre-period breakouts” Window
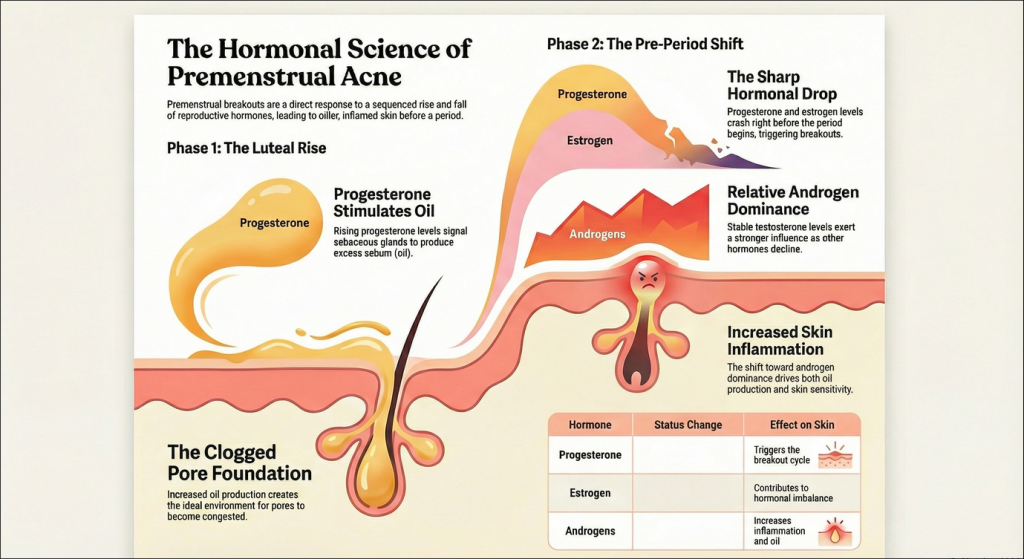
After ovulation your body has entered the luteal phase – progesterone levels surge upwards in this time and one of the effects of that is that it gives a big boost to the sebaceous glands i.e. the oil glands – to produce even more sebum which, while a natural process, can be the final nail in the coffin for people with acne prone skin and just contributes to clogged pores.
As your period gets closer, both progesterone and estrogen levels drop sharply – and its that sudden plummet that is a key trigger for breakouts.
The Role of Androgens: Testosterone’s Relative Increase
While estrogen and progesterone fall, levels of androgens (like testosterone) remain relatively stable. This means that in the days before your period, androgens have a more pronounced effect—a state sometimes called “relative androgen dominance”. Androgens further stimulate oil production and can increase skin inflammation.
It’s not necessarily that you have “high” testosterone; it’s that the balance between hormones shifts, making your skin more responsive to androgens.
Why Your Skin Reacts: Sebum, Pores, and Inflammation
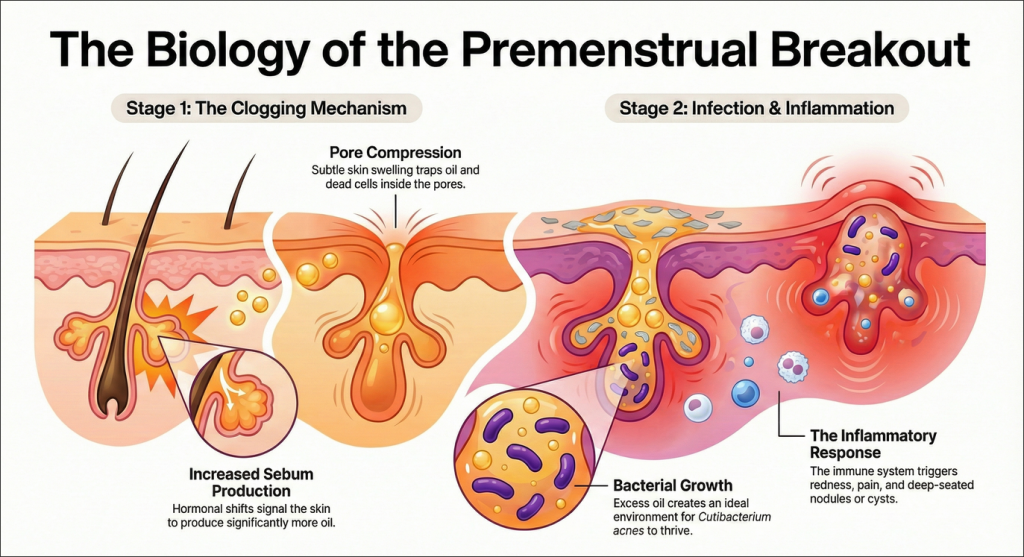
The hormonal shifts of the luteal phase create a perfect storm for acne:
- Increased Sebum Production: More oil (sebum) is produced.
- Pore Changes: Hormonal fluctuations can cause subtle skin swelling, which compresses pores and makes it easier for oil and dead skin cells to become trapped.
- Bacterial Growth: The excess oil creates an ideal environment for Cutibacterium acnes, a bacteria that contributes to acne.
- Inflammation: Your immune system responds to the bacteria and the clogged pore, leading to the redness, swelling, and pain characteristic of inflammatory acne (papules, pustules, nodules, and cysts).
This explains why premenstrual breakouts are often deeper, more tender, and slower to heal than typical blackheads or whiteheads.This chain of events explains why premenstrual acne is often more inflamed and tender.
Why Generic Acne Advice Often Falls Short
Many common acne suggestions you hear – like ‘wash your face more often’ or ‘use a more intense spot treatment’ – just aren’t enough to tackle premenstrual acne because they don’t look for the underlying hormonal cause. Over-washing or using harsh products can wind up stripping your skin of its natural protection, making it red and inflamed, and maybe even worse breakouts.
Likewise, while it’s true that diet, stress, and sleep are involved, they’re not the root of the problem. Stress, for instance, can send your cortisol levels soaring, making hormonal fluctuations even worse. Eating a diet high in sugars can boost inflammation in your body. But even with a perfect lifestyle routine, you can still get breakouts if your hormones shift.
Skincare Adaptations for the Pre-Menstrual Phase
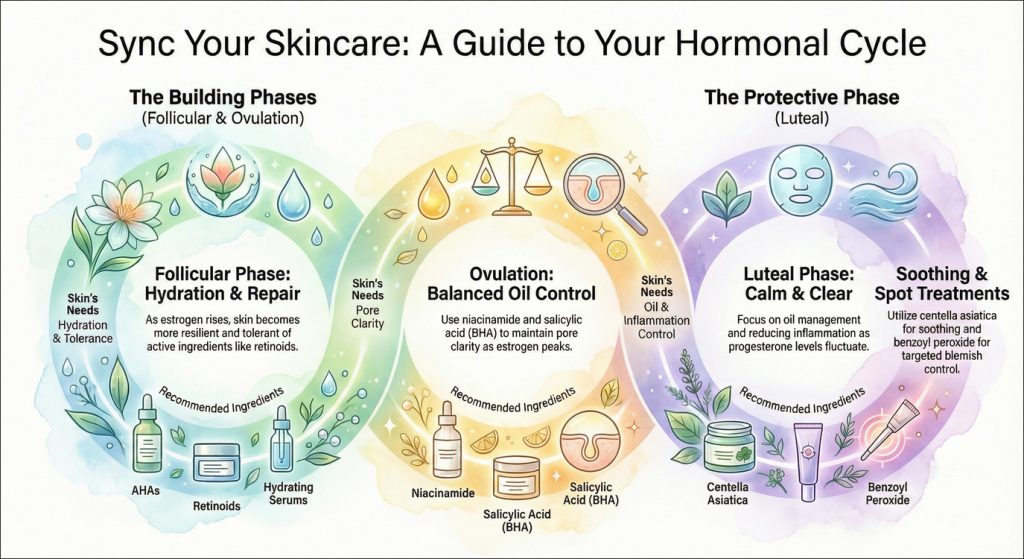
A more effective approach is to align your skincare with your cycle’s phases, supporting your skin’s changing needs rather than fighting them.
| Consistent use of niacinamide and salicylic acid (BHA) for pore clarity. | Hormonal Landscape | Skin’s Needs | Skincare Focus |
|---|---|---|---|
| Follicular Phase (after period) | Estrogen rises; skin is more resilient. | Hydration, repair, and tolerance for active ingredients. | Hydrating serums, gentle exfoliation (AHAs), introducing retinoids if desired. |
| Ovulation | Estrogen peaks; testosterone may also rise. | Balanced oil control and prevention. | Consistent use of niacinamide, salicylic acid (BHA) for pore clarity. |
| Luteal Phase (before period) | Progesterone rises then falls; androgens have relative influence. | Gentle cleansing, oil management, and reducing inflammation. | Oil-free, non-comedogenic products; spot treatments with benzoyl peroxide or azelaic acid; soothing ingredients like centella asiatica. |
Important Note: This supportive framework is really about finding what works best for you and not following some strict set of rules. The key is to get some basic, easy habits in place so you can keep your skin in good health through the ups & downs of life. A simple daily routine of washing your face with a cleanser, moisturizing, and applying some sunscreen will do the trick.
When to Consider Professional Guidance
While premenstrual acne is pretty common, it’s a good idea to get some professional help if your breakouts are getting out of hand. Here are some signs that it might be time to see a doctor or dermatologist:
- You’re thinking about trying something like topical retinoids, birth control, anti-androgens or isotretinoin – these are prescription options that only a doctor or dermatologist can prescribe.
- Your breakouts are bad enough to leave scars, and nothing else is working to calm them down.
- You’ve tried all the usual over-the-counter stuff & taken steps to avoid getting acne when you’re on your period, but you still can’t see any improvement even after a few months.
- You’re dealing with some other symptoms that suggest your hormones might be off-balance – like irregular periods, too much facial or body hair, or unexplained weight gain.
These recurring breakouts can lead to stubborn discoloration — see Red Acne Marks That Won’t Fade: A Guide to Stubborn Discoloration.
Frequently Asked Questions
1. Is premenstrual acne a sign of a hormone imbalance?
Not a sign of an imbalance necessarily – a pretty common response to the hormonal ups and downs of your menstrual cycle. However, if acne is pretty bad or is accompanied by some other pretty unusual symptoms, it’s worth chatting with a doctor to see if there’s something else going on that needs to be looked at.
2. Why does my acne start a full two weeks before my period?
Breakouts around ovulation ( usually about two weeks before the start of your period ) are often linked to that mid-cycle spike in androgens. This can get the oil glands going and before you know it you’ve got a bunch of pimples popping up a few days later.
3. Can birth control pills help with hormonal acne?
Some oral contraceptives have been shown to help by regulating hormone levels and reducing the impact of androgens. They’re actually FDA-approved for acne treatment but do require a prescription and aren’t for everyone – just to warn you . Acne might actually get a little worse before it gets better when you first start.
4. Are there supplements that can help with hormonal acne?
There’s some evidence that certain supplements – like zinc for instance, can help keep your skin healthy and that omega-3 fatty acids might help moderate the level of inflammation in your skin. But let’s be real, supplements are no magic bullet, and its worth talking to a healthcare provider about them to make sure you won’t have any negative interactions or side effects.
5. Is it true that hormonal acne only appears on the jawline and chin?
Yeah, the lower face is a classic place for hormonal acne to show up, but it can appear on the cheeks, neck, back and shoulders too. The exact location will depend on where your oil glands are most sensitive to the hormonal changes
Conclusion
Premenstrual acne is a pretty clear indicator that your hormones are playing a big close-up starring role in the state of your skin. So lets move past all the general advice and get to the nitty gritty of why this is happening – specifically the hormonal ups and downs that come with your monthly cycle. You know, the why behind all the zits popping up. By understanding this side of things, you can start shifting your mindset from feeling stuck and frustrated to actually being able to take care of your skin in a way that works for you.
And remember – it’s unrealistic to expect to banish every last pimple – but with a bit of knowledge, patience and some good old self-care, you can definitely learn to support your skin through its monthly rollercoaster. And if self-care alone doesn’t cut it, that’s where partnering up with a healthcare pro comes in – they can give you access to all sorts of safe and effective options that work.
Disclaimer: This article is for educational purposes only and does not replace professional medical advice. Always consult a healthcare provider or dermatologist for diagnosis and treatment of acne or any skin condition.