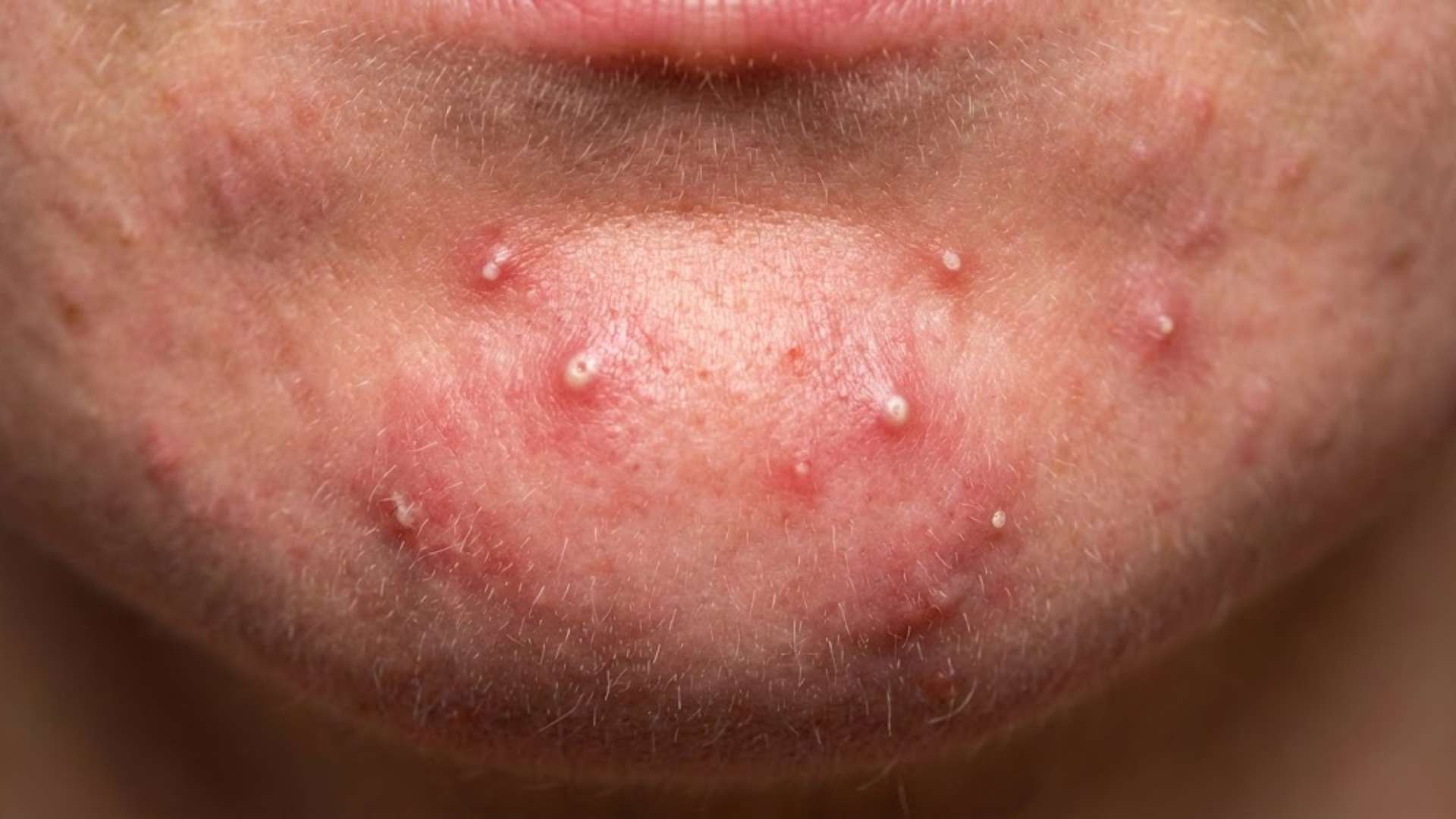
If you’ve ever had a deep, tender pimple on your chin that seems to appear out of nowhere, you know it’s a uniquely frustrating experience. Unlike surface blemishes, these pimples are often painful to the touch and can linger for weeks. While commonly associated with teenage years, they frequently persist into adulthood, particularly affecting women due to hormonal fluctuations.
This article explains why the chin is a common site for these painful breakouts, distinguishes the different types you might encounter, and outlines a clear, practical approach for caring for your skin. Our focus is on providing you with a deeper understanding of the processes beneath your skin, which is the first step toward making informed, effective decisions about your skincare.
Some painful chin breakouts are actually deep cystic lumps — learn more in Hard Painful Lump Under Skin on Chin: Causes and Care Explained.
Why the Chin? The Anatomy of a Painful Pimple
To understand chin pimples, it’s helpful to know what’s happening beneath the surface. All pimples begin when a hair follicle, or pore, becomes clogged with a mix of excess sebum (skin oil) and dead skin cells. This creates an ideal environment for Cutibacterium acnes, a bacteria that lives on skin, to multiply, leading to inflammation, redness, and swelling.
The chin, along with the jawline and lower cheeks, is rich in sebaceous glands that are highly sensitive to hormones, particularly androgens like testosterone. These hormones stimulate the glands to produce more oil. This is why breakouts in this “beard distribution” area are so often linked to hormonal cycles—such as during the menstrual cycle, pregnancy, menopause, or times of significant stress.
Furthermore, the pimples that form here tend to be deeper and more inflamed. When the clog and resulting inflammation occur deep within the hair follicle in the skin’s dermis layer, it forms a nodule or cyst. These are the painful, often hard bumps you can feel under the skin long before you see a head. They are more likely to cause scarring because the inflammatory damage occurs at a deeper level of skin tissue.

| Type | What It Is | Characteristics |
|---|---|---|
| Papule | An inflamed, clogged pore. | Small, pink or red, raised bump; can be tender. |
| Pustule | A papule with pus at its surface. | Red base with a visible central white or yellow head. |
| Nodule | A deep, solid clog and inflammation. | Large, hard, painful lump deep under the skin; no visible head. |
| Cyst | A deep, pus-filled clog and inflammation. | Large, painful, pus-filled lump deep under the skin; can cause scarring. |
A Practical Approach to Care and Management
Managing painful chin acne requires patience and consistency, as results from most treatments take four to eight weeks to become apparent. The goal is to reduce inflammation, prevent new clogs, and support the skin’s healing without causing further irritation or damage.
Foundational Skincare Practices
Consistent, gentle care forms the bedrock of management:
- Cleanse Gently: Wash the area twice daily with a mild, non-abrasive cleanser and lukewarm water. Avoid harsh scrubs or vigorous washing, which can worsen irritation.
- Use Key Active Ingredients: Look for over-the-counter products containing proven ingredients. Apply a thin layer to affected areas as directed.
- Moisturize and Protect: Use a light, oil-free, non-comedogenic moisturizer. Daily sunscreen (also non-comedogenic) is crucial, as some acne treatments and inflammation itself can increase sun sensitivity and the risk of dark spots.
- Hands Off: It is critical to resist picking, squeezing, or popping these pimples. This forces bacteria deeper, dramatically increases inflammation, and significantly raises the risk of infection and permanent scarring.
Recurring chin acne is often hormone-related — explained in Why Does Acne Get Worse Before Your Period?
| Ingredient | Primary Action | Notes |
|---|---|---|
| Benzoyl Peroxide | Kills acne bacteria and helps clear pores. | Can cause dryness or bleaching of fabrics. Start with a lower concentration (2.5-5%). |
| Salicylic Acid | Exfoliates inside the pore to prevent clogs. | A beta-hydroxy acid (BHA) good for blackheads and whiteheads. |
| Adapalene | A topical retinoid that prevents clogged pores. | Now available over-the-counter. Promotes cell turnover; can cause initial dryness. |
| Azelaic Acid | Fights bacteria and reduces inflammation. | May also help improve post-acne discoloration. |
Supportive At-Home Measures
For an acute, deep pimple, dermatologists recommend a warm compress. Apply a clean, warm, damp cloth to the area for 10-15 minutes, three times a day. This can help encourage the pimple to come to the surface and resolve. Hydrocolloid acne patches can also be helpful for pimples with a surface head, as they protect the area, absorb excess fluid, and prevent picking.
Some natural ingredients have supporting research. For example, tea tree oil has antibacterial and anti-inflammatory properties. One study found a 5% tea tree oil gel was effective, though it may work more slowly than benzoyl peroxide. It must always be diluted with a carrier oil (like jojoba) before application to avoid severe irritation. Green tea extracts, applied topically, have also shown anti-inflammatory benefits in studies.
When Self-Care Isn’t Enough: The Role of Professional Help
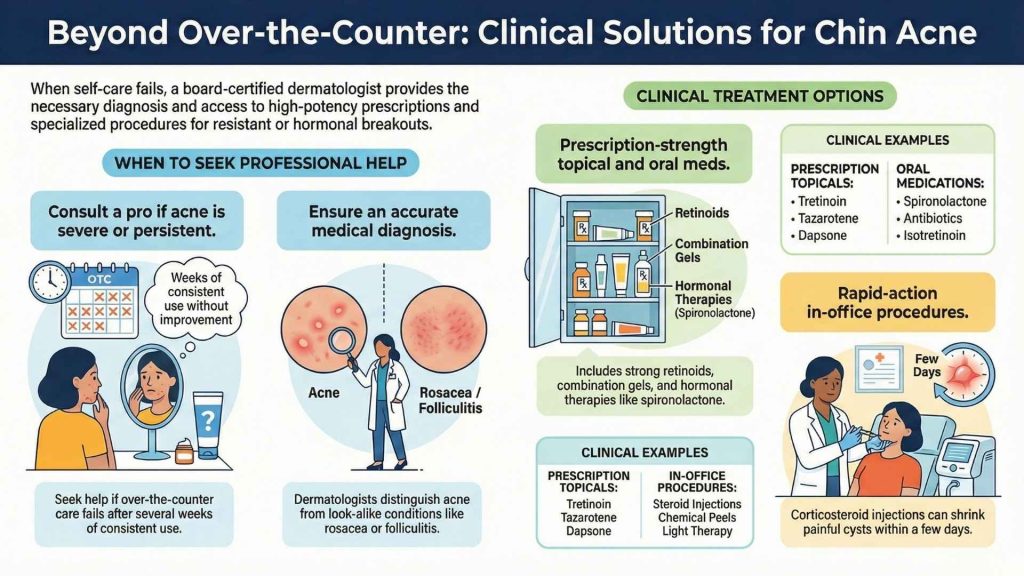
If painful chin pimples are frequent, severe, or do not respond to several weeks of consistent over-the-counter care, it is time to consult a board-certified dermatologist. They can provide accurate diagnosis (sometimes what looks like acne can be rosacea or folliculitis) and access to prescription-strength treatments.
Prescription topical treatments include stronger retinoids (tretinoin, tazarotene), combination antibiotic/benzoyl peroxide gels, or dapsone. For deeper hormonal acne, oral medications may be recommended. These can include oral antibiotics for inflammation, hormonal therapies like certain birth control pills or spironolactone (which blocks androgen effects), or isotretinoin for severe, resistant cystic acne.
Also Read : Skin-Colored Bumps on Forehead ? Find Your Solution Here.
Dermatologists also offer in-office procedures. A corticosteroid injection can rapidly shrink a large, painful cyst, reducing pain and inflammation within days. Other options like chemical peels, light therapy, or professional drainage may be part of a comprehensive treatment plan.
Lifestyle and Holistic Considerations
While not direct causes, certain lifestyle factors can influence hormonal balance and inflammation, potentially affecting breakouts.
- Diet: Emerging research suggests a possible link between high-glycemic diets (rich in sugary, processed foods) and dairy intake with increased acne severity for some people. A balanced diet rich in whole foods, vegetables, and omega-3 fatty acids may support overall skin health.
- Stress Management: Chronic stress elevates cortisol levels, which can stimulate oil production. Incorporating stress-reducing activities like adequate sleep, exercise, or meditation can be a beneficial component of skin care.
- Product Management: Ensure all products that touch your face—including makeup, sunscreen, and even phone screens—are non-comedogenic and oil-free. Regularly clean items like pillowcases, phone, and glasses.

Frequently Asked Questions
While not exclusively hormonal, recurrent, deep pimples along the chin, jawline, and lower cheeks are a classic pattern of hormonal acne. This is because the oil glands in this area are particularly sensitive to androgen hormones. If breakouts coincide with your menstrual cycle or occur alongside other symptoms like irregular periods, consulting a doctor or dermatologist is wise.
The relationship is complex and individualized. Rigorous scientific consensus is still evolving, but some studies indicate that for some people, diets with a high glycemic load (lots of sugars and refined carbs) and high dairy intake may exacerbate acne. It’s not about one food causing a pimple overnight, but rather the potential for dietary patterns to influence inflammation and hormone levels over time.
Stress triggers the release of hormones like cortisol. Elevated cortisol can increase your skin’s oil production and amplify inflammation throughout the body, creating an internal environment more prone to breakouts. Furthermore, stress can lead to behaviors like picking at skin, which worsens existing pimples.
Dermatologists uniformly advise against it. Deep nodules and cysts are walled off under the skin. Attempting to pop them often ruptures the lining, spreading inflammation deeper and causing more damage, which significantly increases the risk of scarring and infection. If a pimple absolutely must be drained, it should be done by a medical professional under sterile conditions.
With proper care, a standard pimple may resolve in a few days to a week. However, deep nodules or cysts exist far beneath the surface and have a much longer inflammatory cycle. It is not uncommon for them to last for several weeks, or even a month or more, to fully resolve. Consistency with treatment is key.
Conclusion
Painful chin pimples are more than a surface nuisance; they are a sign of deep-seated inflammation often tied to hormonal activity. Effective management combines gentle, consistent skincare with scientifically backed active ingredients, a focus on non-irritation, and an understanding of supportive lifestyle factors. Most importantly, recognizing when to seek professional dermatological guidance is crucial for preventing scarring and addressing persistent or severe cases. By focusing on understanding the underlying causes and responding with patient, informed care, you can navigate these breakouts with greater confidence and clarity.
Disclaimer: This article is for educational purposes only and does not replace professional medical advice. Always consult with a board-certified dermatologist or healthcare provider for diagnosis and personalized treatment of skin concerns.