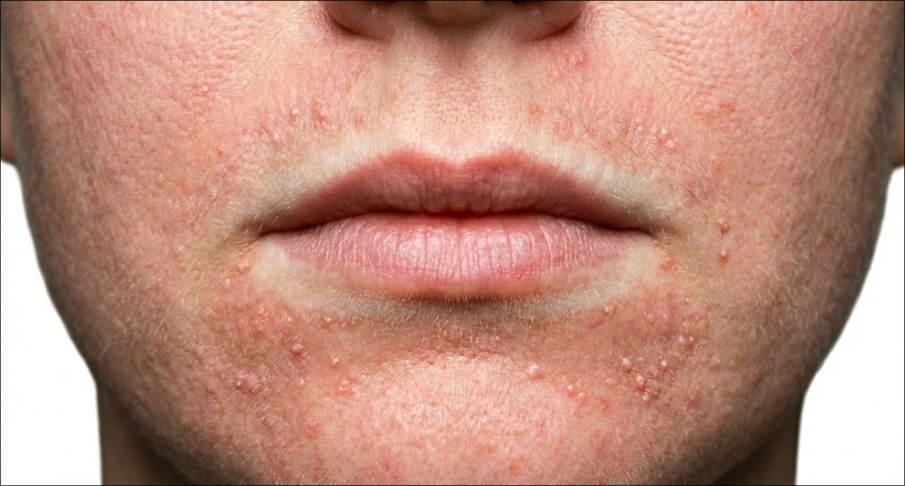
Discovering a cluster of small red or flesh coloured bumps round your mouth can be super confusing and pretty frustrating. These bumps often look suspiciously like pimples, but they can feel different – possibly itchier, tighter or just plain more annoying than a standard pimple.
And if your usual acne fights – face washes or creams – have done absolutely nothing to help, or even somehow made things worse – you’re definitely not alone in feeling stumped. This particular pattern of irritation isn’t acne – it’s a pretty common skin condition called perioral dermatitis.
This article will try to help make sense of what you’re seeing, explain why throwing the usual acne-fighting products at it might not be the best idea, and go over some common triggers and patterns that can come up with perioral dermatitis. Our aim is to give you some real clarity, so you can make more informed decisions about your skin care. If your redness comes with sudden warmth or blushing, read:
Skin Flushing: What It Is, Causes & Treatment.
The First Clue: What Makes This Rash Different
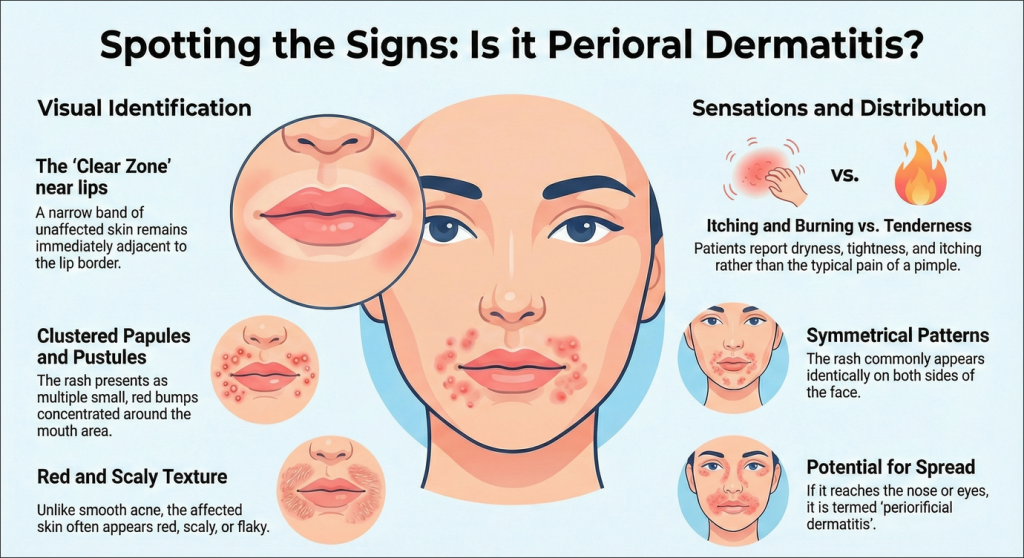
While its easy to just lump all facial bumps together as “acne”. Perioral dermatitis however has several telltale characteristics that set it apart. It normally shows up as a bunch of small bumps or pustules clustered right around the mouth along with a couple of other pretty distinctive signs. And one of those is that the rash usually leaves a clear little zone just right next to where your lips meet the skin, that remains completely unaffected.
Beyond where it shows up, the sensation people get from it is often different too. Lots of people report what they’d describe as feeling of dryness, or a tight, itchy, or even a sort of mild burning sensation – which is really different from the tenderness of a pimple. The skin over the top of the rash can be red, flaky, or scaly looking. And also it’s pretty common for the rash to show up on both sides of the face at the same time – and in some cases it can even spread out to the area around the nose and sometimes even the area around the eyes. When this happens, its called periorificial dermatitis.
Why Standard Acne Advice Often Fails Here
Its pretty maddening when treatments that used to get rid of breakouts have zero effect for perioral dermatitis – or worse still, make things even worse. The thing is, the underlying problems are just fundamentally different.
- Acne – it’s a hair follicle & oil gland issue really. Clogged pores, too much oil, and some nasty bacteria ( you know, C. acnes) are the main culprits. Stuff like benzoyl peroxide and salicylic acid is supposed to get the pores unclogged, reduce the oil and kill off the bacteria.
- Perioral Dermatitis though is an entirely different ballpark – its an inflammatory reaction in the skin, usually linked to issues with the skin barrier and your body’s immune response getting over-enthusiastic. Its not about clogged pores like with acne, so trying to clear them out isnt going to solve anything. Which is why all those harsh acne treatments can just make your skin barrier even worse off, which in turn makes things even more inflamed and slows down healing.
And then theres the often-seen (but not really helpful) reaction of slapping on an over the counter hydrocortisone cream to try and sort out the dryness & redness. Yeah, it might give you temporary relief but before you know it, you can end up in a vicious cycle of needing to rely on it all the time, and the moment you stop using it you get another flare-up – which is actually a key thing that sets off the condition to start with.
Understanding Perioral Dermatitis: A Different Kind of Inflammation
The exact cause of perioral dermatitis is not fully understood, but it is widely recognized as a multifactorial condition. It occurs when the skin’s natural barrier function is disrupted, leading to increased sensitivity and perivascular inflammation (inflammation around small blood vessels). Think of it as your skin’s immune system becoming overly reactive to various triggers it once tolerated.
Struggling to build the right routine to prevent flare-ups? Start here:
Morning vs. Night Skincare: What’s the Difference?
The Primary Suspect: Topical Steroids and the Rebound Effect
The most well-documented trigger is the use of topical corticosteroid creams on the face. This creates a paradoxical cycle:
- A steroid cream is applied (often for a separate issue like mild eczema or what is mistaken for acne).
- It suppresses inflammation, making the initial redness and bumps appear to improve.
- With continued use, the skin becomes dependent on the steroid.
- Upon stopping, the skin experiences a rebound flare that is often worse than the original condition, prompting the user to reapply the steroid.
This cycle can be initiated even by low-potency, over-the-counter hydrocortisone used for more than a short period. Inhaled steroids (from asthma inhalers) and nasal steroid sprays can also contribute if residue comes into contact with facial skin.
Common Aggravating Factors
A range of other factors can initiate or worsen perioral dermatitis in susceptible individuals by irritating the skin or disrupting its microbiome:
- Heavy Skin Care Products: Thick creams, ointments, and oil-based foundations can occlude (block) the skin, trapping heat and bacteria and potentially fueling inflammation.
- Certain Oral Care Ingredients: Fluoride and the foaming agent sodium lauryl sulfate (SLS) in toothpaste are frequent irritants for the delicate perioral skin.
- Physical Factors: Chronic moisture from lip-licking, drooling (in children), or occlusive gear like face masks can create a disruptive environment for the skin barrier.
- Other Potential Triggers: Hormonal fluctuations, certain cosmetic ingredients, and even immune system variations may play a role.
Patterns That Help: Calming Over Cleaning The Clusters Around Mouth
Managing perioral dermatitis is all about ditching that “all-out attack” mentality. Switching to a more laid-back approach calm, gentle and repair-focused.
The Less-Is-More Skincare Strategy
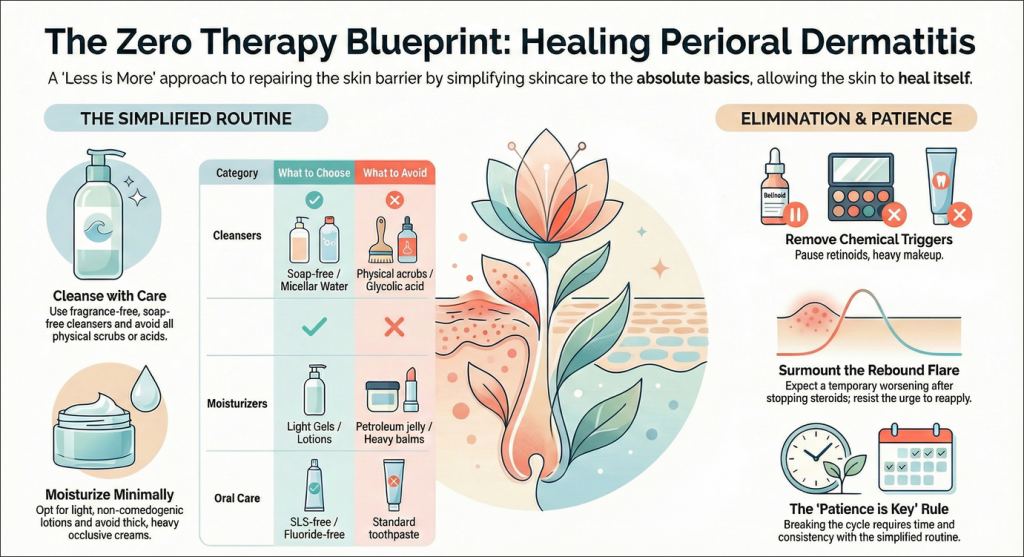
The one step that’s most likely to make a big difference is paring down your skincare routine to only the most non-irritating products. This is sometimes called a “skin detox” or “zero intervention” – the bare essentials.
- Cleanse Gently: Use a cleanser that doesn’t contain any nasties: no fragrances, no soap. You can try a micellar water for a super simple option. Leave the scrubbing and harsh exfoliating acids (like glycolic or salicylic acid) to the unaffected areas.
- Get Minimal Moisturising Going On: If you really need to, just go for a light, non-greasy moisturiser that won’t clog pores, and skip the thick balms and heavy creams.
- Identify and Ditch the Triggers: Think about switching to a toothpaste that doesn’t contain SLS or fluoride, and make sure to get all the toothpaste out of your mouth when you’re done brushing. Give your active skincare products (retinoids, vitamin C, etc) and heavy makeup a break for a bit.
- Keep Your Cool: When you stop using steroid creams, the rash might actually get a little worse (that’s a rebound flare) before it starts to get better – so try to be patient and not go back to the steroid.
When to Seek a Professional Help For Clusters Around Mouth
If you’ve cut back on your skincare routine and still aren’t seeing any improvement after a few weeks, or if the condition is pretty bad, get in touch with a healthcare pro – it can make a big difference. A dermatologist is the right person to be talking to. Perioral dermatitis can look a lot like rosacea, contact dermatitis, or even just plain old acne.
A professional can really help you out with things like:
- Gels and Creams from the Doctor’s Office: They can prescribe non-steroid creams. Like metronidazole, azelaic acid or pimecrolimus to help calm things down.
- Pills from Your Doctor: If the condition has spread a bit, you might be put on some oral antibiotics. Something like doxycycline or minocycline. An important thing to remember is that they’re being used to reduce inflammation – not because you’ve got an infection.
- Getting Some Real Expert Advice: A pro can help you wean yourself off those topical steroids. If you’ve been using them. Come up with a long-term plan to keep your skin looking good and prevent things from coming back.
Frequently Asked Questions
If whatever’s triggering it gets sorted out then the rash might start to heal all by itself. But don’t expect it to be a quick fix. It could take anywhere from weeks to months to clear up. Stopping steroids in particular can lead to a nasty rebound flare that’s hard to deal with.
No not usually. Sure, an overgrowth of the usual skin bugs might be playing a part. But perioral dermatitis isn’t an infectious disease itself. So you don’t have to worry about catching it from someone else.
Diet does not bring on perioral dermatitis – research has not shown that any one food starts the rash. Acid or spice sometimes reddens skin that is already fragile. But the main provocation comes from what touches the face, not from meals.
Hormonal acne differs from perioral dermatitis – hormonal lesions sit deeper and feel cystic. They gather along the jaw plus chin and return with the monthly cycle. Perioral dermatitis shows many small, surface level red papules that itch or scale.
What You May Also Ask
No, thankfully, perioral dermatitis isn’t anything you’ve got to live with permanently. But it can be a bit of a tricky customer. If you don’t sort out the things that are making it worse, it can stick around & come back. So you’ll need to nail down what’s causing it & take good care of your skin.
As well as topical steroids being a major trigger, there are plenty of other things that can set off your skin. Like ingredients in your skincare or makeup, or even your toothpaste.
Conclusion
Those pesky little pimple clusters around the mouth are a whole different ball game compared to your average acne. Getting to the root of perioral dermatitis means being able to spot it – its telltale location, how it feels, and just how badly it reacts to run of the mill treatments. You have to grasp that its all about the inflammation – and take the necessary time to figure out what’s causing it, probably a corticosteroid cream or harsh product, and put your skincare routine in low gear – lots of calming ingredients, you know the drill. If home remedies don’t do the trick, time to pay a visit to a dermatologist – they’ll show you the smart way to tackle it with targeted anti-inflammatory treatments.
Disclaimer: This article is for educational purposes only and does not replace professional medical advice. It is not intended to diagnose or treat any condition. If you have concerns about your skin, please consult a healthcare professional such as a dermatologist.