Do you ever suffer from those occasional concerns about your breath? You do all the right things, following all the typical advice (brushing, flossing, chewing gum), and yet the feeling — or worse, a comment from someone nearby — persists. Chronic bad breath — one that never seems to go away no matter how much you brush or pop a mint (or five) — is more than an occasional social downside.
For some people, it’s something they deal with every single day, and feel like there’s nothing that can solve it. It’s the distance between doing what you believe to be right and not getting the outcome you hope for.
This article will guide you through why standard fixes might fail and what complex factors could be at play, helping you move from frustration to understanding. If you’re noticing white debris in the back of your throat, check White Chunks in Throat that Smell Bad: The Protocol.

Why This Feels Different
First off, we have to differentiate between transient and persistent bad breath. Morning breath, garlic breath or “coffee mouth” are typically addressed with a rinse and spit. Chronic halitosis is different. It’s the smell that seems to return moments after you brush your teeth, feels like it arises from deep in your throat and even after you stop smoking, it won’t go away, or has a pungent scent that mints can’t cover. That persistence is your body’s way of saying that the source might be more than just some crumbs from dinner.
The Science of Smell: It’s Usually About Bacteria
To figure out why bad breath is so persistent, we have to begin with its most frequent producer — volatile sulfur compounds (VSCs). These are gases made by certain bacteria that already live in your mouth. These bacteria feed on proteins in food remnants, dead skin cells, and mucus, creating smelly byproducts like hydrogen sulfide (rotten eggs) and methyl mercaptan (rotting cabbage).
The bacteria are kept in check by a healthy oral environment. Problems arise when certain conditions allow these odor-producing bacteria to overpopulate or thrive in areas that routine cleaning misses.
Where Standard Advice Falls Short: Looking Beyond the Basics
Telling someone with chronic bad breath to “brush better” is often unhelpful. They usually are brushing—perhaps obsessively so. The issue is that the source of the odor may be in locations that a toothbrush can’t easily reach or may be linked to factors beyond just cleaning.
Here are key areas where standard routines may not reach:
- The Back of the Tongue: The leading culprit of chronic bad breath. The surface of the tongue, particularly the back 1/3, is pitted with small crevices and papillae. This leaves a large, low-oxygen environment in which bacteria can grow undisturbed. Running a brush quickly across the front of your tongue does little to disrupt this ecosystem.
- Beneath the gumline (periodontal pockets): If gums are inflamed or even receding slightly from teeth (the hallmark of gingivitis or periodontitis), they’ll also create pockets. These pockets also provide reservoirs for detrimental bacteria, which produce VSCs. Flossing can clean between teeth, but it cannot always penetrate the bottom of these infected pockets.
- The Tonsils (Tonsil Stones): The tonsils have holes known as crypts. Garbage like food, mucus and dead cells can become caught and solidify into yellowish, stinky little fluorescent nuggets known as tonsil stones or tonsilloliths. This can lead to a lasting bad taste in the mouth and larynx, and it can cause symptoms such as throat clearing.
- A Chronic Dry Mouth (Xerostomia): Saliva is God’s mouthwash. It is a neutralizing acid, washes away debris, and has antiseptic enzymes built in. Reduced saliva flow—from medications, breathing through the mouth, certain health conditions, or simply not drinking enough water—creates an environment where odor-causing bacteria flourish.
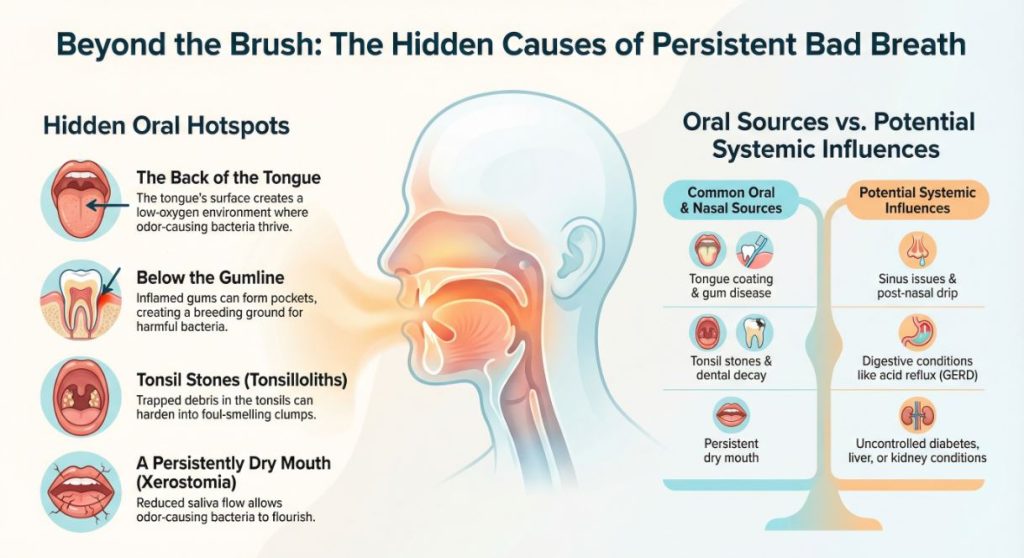
When the Source Isn’t (Only) the Mouth
While most bad breath originates orally, persistent cases can sometimes be influenced by other factors. It’s crucial to understand these, not to self-diagnose, but to have an informed discussion with a healthcare professional.
| Common Oral & Nasal Sources | Potential Systemic Influences |
|---|---|
| Tongue coating (bacteria on the back of the tongue) | Sinus & respiratory issues (chronic post-nasal drip feeds mouth bacteria) |
| Gum disease (gingivitis, periodontitis) | Digestive conditions (like chronic acid reflux/GERD) |
| Tonsil stones (debris in tonsil crypts) | Uncontrolled diabetes (can cause a distinctive fruity or acetone smell) |
| Dental issues (decay, ill-fitting crowns, dirty dentures) | Liver or kidney conditions (can alter breath odor) |
| Persistent dry mouth (from meds, lifestyle, or conditions) |
Navigating the Social and Emotional Impact
The experience of halitosis often carries a profound impact on self-esteem and relationships. People may become less talkative, feel insecure, and experience strain in intimate relationships where partners are afraid to bring it up. This anxiety can create a vicious cycle, as stress itself can worsen dry mouth and oral issues.
If you have to discuss this with a loved one, concentrate on health and care, not blame. Use “I” statements, and convey concern: “I’ve noticed something that appears to be persistent, and I care about your health. Have you considered speaking with a dentist to see if maybe there is some kind of underlying cause? This is a better approach than an adversarial one.
A persistent white tongue coating may also be contributing — learn more in White Coating on Tongue? Stop Scraping (The Real Fix).
When to Seek Professional Guidance: Drawing the Line
This is the most critical step. You should schedule an appointment with a dentist or dental hygienist if:
- The bad breath persists despite consistent, improved oral hygiene for two weeks.
- You notice signs of gum disease (bleeding, redness, swollen gums, or loose teeth).
- You can see a white coating on the back of your tongue or suspect tonsil stones.
- You have persistent dry mouth.
Get an oral health checkup at a dentist’s office. They will measure pockets, find tonsil stones and use instruments to check for VSC. If a cause in your mouth isn’t found, they can send you to the doctor for an investigation into possible sinus, digestive or other systemic causes.
What a Professional Assessment Might Involve
A dental visit for halitosis goes beyond a standard checkup. The professional may:
- Conduct an Organoleptic Assessment: This is the “sniff test,” considered the gold standard, where the dentist rates breath odor at different distances.
- Use a Halimeter: This device measures the concentration of volatile sulfur compounds in your breath.
- Perform a Tongue Coating Index: Assessing the thickness and area of coating on your tongue.
- Check for Periodontal Pockets: Using a probe to measure gum health around each tooth.

What You Can Do: A Stepwise Approach
- Optimize Your Home Care:
- Brush + Floss: Brush twice daily with fluoride toothpaste and floss thoroughly to remove plaque between teeth.
- Clean Your Tongue: Gently but thoroughly clean your tongue daily with a tongue scraper or toothbrush. Focus on reaching the back.
- Hydrate: Drink water consistently throughout the day to support saliva flow.
- Use Alcohol-Free Mouthwash: Alcohol can dry the mouth. Opt for a therapeutic mouthwash with ingredients like cetylpyridinium chloride (CPC).
- Seek Professional Diagnosis: Don’t guess. Let a dentist identify the source—be it deep gum pockets, significant tongue coating, or tonsil stones. They can provide a professional cleaning that removes tartar you can’t.
- Follow Professional Treatment Plans: This may include deep cleaning (scaling and root planing) for gum disease, guidance on managing dry mouth, or referral to a doctor or ENT specialist for tonsil stones or sinus issues.
Frequently Asked Questions
Can bad breath come from my stomach?
Most odors come from the mouth; less often, they originate in the chest and digestive tract, which is a little harder to control. Backwash: Acid from the stomach comes up into your esophagus and begins to corrode; it’s what we taste when we burp, and in high quantities, affects breath. Yet, “stomach breath” is not as prevalent as people think and comes with other symptoms such as heartburn.
I brush and floss constantly. Why isn’t it working?
This is the core frustration. You may be missing the primary source. Over-brushing can even harm gums. The issue is likely in an area you’re not effectively cleaning (like the back of the tongue) or is a condition like early gum disease or tonsil stones that requires professional attention.
Is mouthwash the solution?
Mouthwash is a temporary mask, not a cure. Therapeutic rinses can help reduce bacteria for a short time, but they do not remove the biofilm (plaque) where bacteria live. They are an adjunct to, not a replacement for, mechanical cleaning.
Could it be my tonsils?
Yes. Tonsil stones are a common and overlooked cause. Signs include a persistent bad taste, a feeling of something stuck in your throat, and visible white/yellow spots on your tonsils. An ENT doctor or dentist can diagnose this.
My partner has bad breath. How can I tell them without hurting their feelings?
Choose a private, calm moment and frame it with care and concern for their health, not as a personal critique. Offer to support them in finding a solution, like booking a dental checkup together.
Finding a Path Forward
Chronic bad breath is a complex and frustrating problem, but one that can almost always be controlled once the true source is discovered. The answer isn’t to work harder with the same tools; it’s to work differently. Stop chancing with your health and move on to professional exploration and focused treatment. Once you identify the cause and get the right advice, then you’ll be able to treat the actual issue and not just manage a symptom, which means permanent fresh breath and newfound confidence.
Disclaimer: This article is intended for educational purposes only and does not replace professional medical advice or oral care. Please refer to a professional dentist, physician or other appropriate health professional for diagnosis and treatment of your dental or medical concerns.