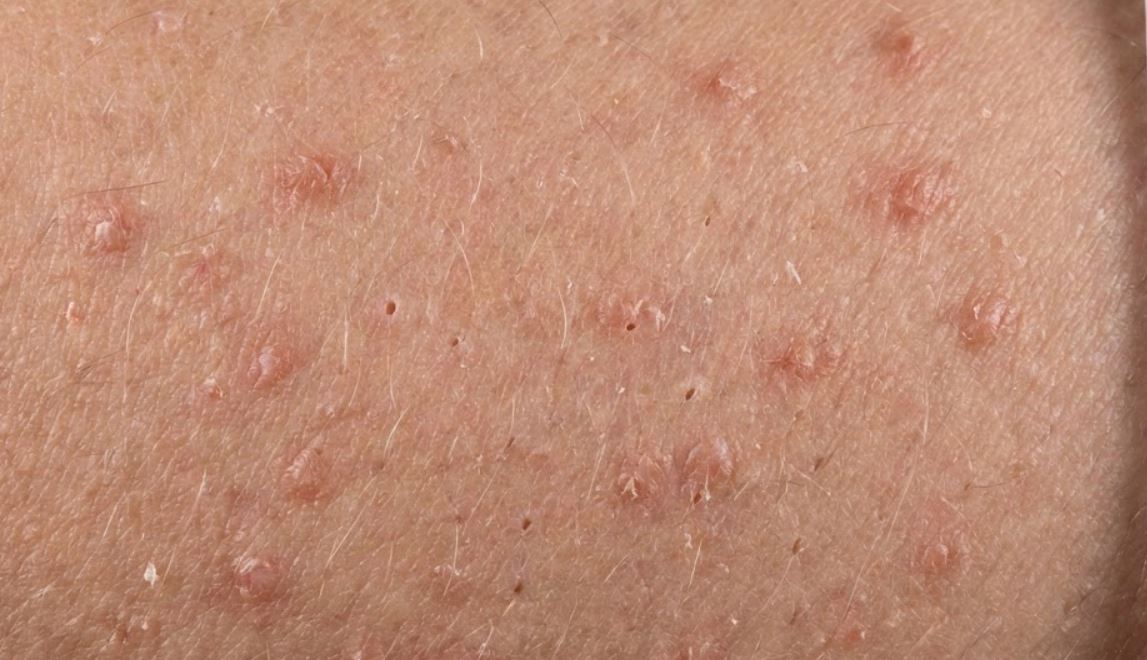
Most people have noticed the appearance of tiny, rough-feeling bumps on the backs of their upper arms. These bumps may be skin colored, red, or brown. It’s ‘feel like having the skin of a porcupine or like ‘permanent sandpaper on my arms’. For many, it’s been that way forever.
And the skin will be “sandy,” something a lot of dermatologists see as KP (short for Keratosis pilaris). It should be noted that keratosis pilaris is a harmless, not an infectious, skin condition. ItÂ’s not contagious, and itÂ’s also not a symptom of any other underlying health condition for the majority of sufferers.
This article intends to provide a simple one-page health education regarding what keratosis pilaris is. And how it can be treated, and … Summary statements on the use of UV radiation for indoor tanning practices. For more on body skin texture, visit: Understanding Loose Stomach Skin: Causes & Care Options
What People Typically Notice About These Bumps
The experience of keratosis pilaris is primarily tactile and visual. People often report:
- Texture: The skin feels consistently rough or bumpy to the touch, regardless of visible redness.
- Appearance: Tiny, pinpoint bumps that may be the same color as your skin or take on a pink, red, or brownish hue, particularly in individuals with darker skin tones.
- Location: A strong predilection for the backs of the upper arms. It can also appear on the thighs, cheeks, or buttocks.
- Behavior: The bumps and bumpy texture might seem more apparent or feel drier in the colder months when there is less humidity, and skin may lose moisture. Some see fluctuations with hormonal changes.
- Feeling: This usually doesn’t hurt or itch for most people, but some may have mild to moderate itching.
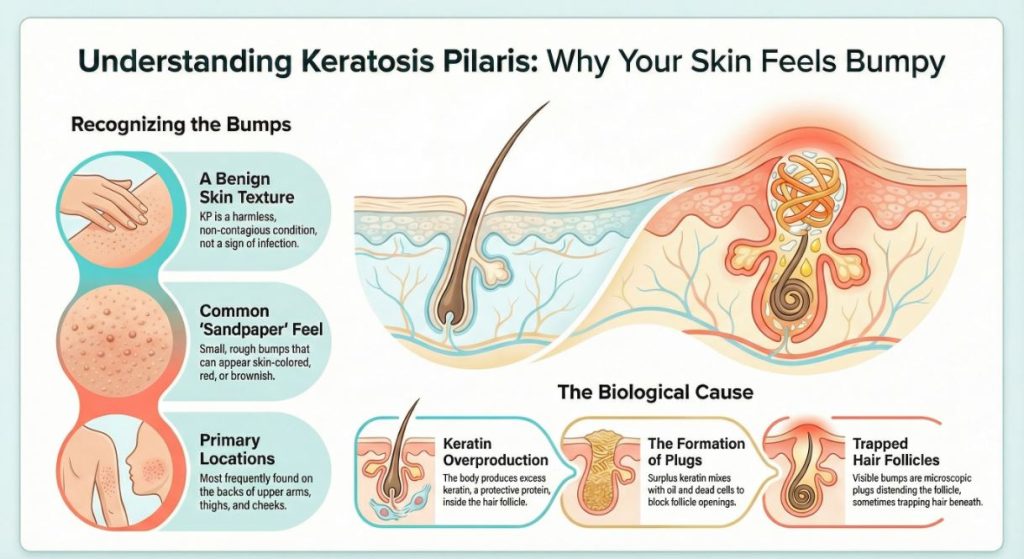
The Underlying Mechanism: Why KP Happens
To understand keratosis pilaris, it helps to visualize a hair follicle—the tiny opening from which a hair grows. Inside the follicle, a hair is surrounded by skin cells (keratinocytes) that normally shed and renew.
In skin with a tendency for KP, this process becomes altered. An excess amount of a protective protein called keratin is produced. Instead of shedding evenly, this surplus keratin mixes with skin oils and dead skin cells, forming a tiny, firm plug that blocks the opening of the hair follicle. The hair may become trapped beneath this plug or grow alongside it.
To elaborate, what you are observing or feeling as the “bump” is this tiny speck (which is known as a hyperkeratotic plug) lodged within and expanding the hair follicle. The redness or pigmentation present about the bump is often from a minor inflammatory response, which is caused either by the foreign material or by the hair follicle itself.
Key Factors Influencing KP Development
The inclination to keratosis pilaris is thus most likely predominantly transmitted genetically. Their children, if one or both parents have it, are also more likely to have it. It’s frequently associated with other skin issues like atopic dermatitis (eczema) or very dry skin (xerosis).
Apart from genetic causes, there are many internal and external factors that determine their prominence. If you use self-tanner, don’t miss: Understanding Self-Tanner Streaks on Elbows and Knees
| Shaving (as a cause): Shaving can irritate existing KP, but doesn’t initiate it. | Often Misunderstood as Triggers |
|---|---|
| Genetic Predisposition: A family history of KP, eczema, or asthma. | Poor Hygiene: KP is not caused by dirt and cannot be scrubbed away. |
| Naturally Dry Skin: An impaired skin barrier loses moisture easily. | Dietary Choices (Directly): No consistent evidence links specific foods to causing KP for most. |
| Natural Hormonal Shifts: Often appears in childhood, may flare in puberty, and can change during pregnancy. | Shaving (as a cause): Shaving can irritate existing KP but doesn’t initiate it. |
| Environmental Conditions: Low-humidity climates (winter) or frequent hot baths can exacerbate dryness. | Infections: It is not bacterial, viral, or fungal. |
| Skin Barrier Disruption: Using harsh soaps or over-exfoliating can worsen the underlying dryness. |
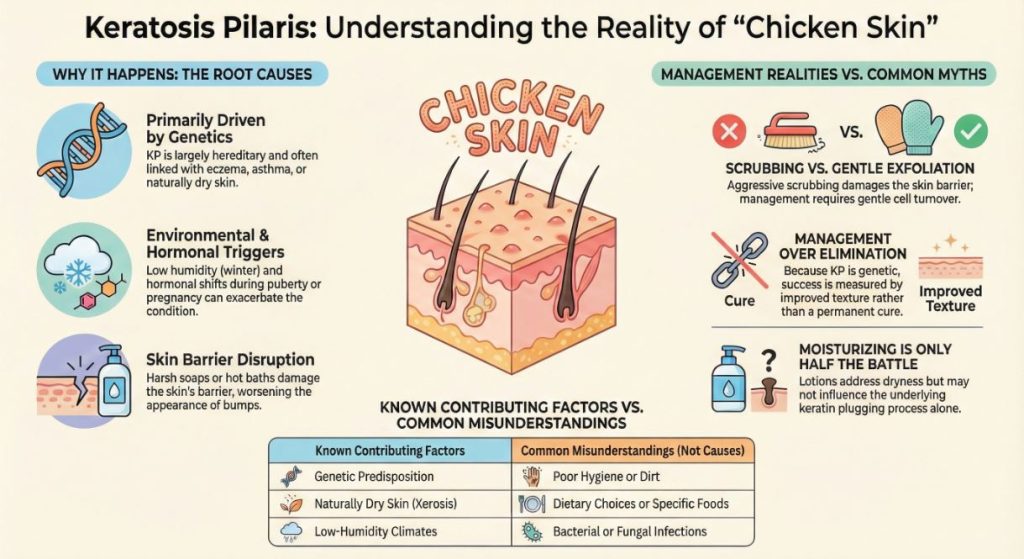
Why Common Skin Care Advice Can Feel Confusing or Ineffective
Many individuals seeking smoother skin turn to standard exfoliation or moisturizing routines. When results are inconsistent or temporary, it can lead to frustration. Here’s why generic advice may fall short for keratosis pilaris:
- Misconception: Scrubbing harder. Using physical scrubs, or a rough loofah, to “buff” away the surface of keratin plugs will give you an immediate smoothness. Though this can be achieved not by dissolving the plugs, but shearing off their tops. But this aggressive treatment can also damage the fragile skin barrier around your follicles, making them even drier and more irritated — and potentially inflamed (which means those bumps seem redder). The respite is only skin deep and temporary.
- Moisturizing Alone Isn’t Always Enough: While crucial, applying a basic lotion addresses the dryness associated with KP but doesn’t directly influence the keratin plugging process. Effective approaches often combine moisture with ingredients that gently influence cell turnover.
- The Myth of a Lasting “Cure”: Due to the condition being related to some inherited skin features, most people focus on either removal or controlling it rather than “curing” it altogether. Treating KP as a condition to be “cured” can easily result in high, unfeasible standards of achievement. Progress is evaluated by better texture and lessening of the appearance, not eradication.
- Individual Variability: What significantly helps one person may offer only minor improvement to another, due to differences in skin type, the severity of KP, and other individual factors.
Patterns of Care That Users Often Report as Supportive
Schools of thought and people who attend various meetings of like-minded individuals make up for the patterns that bubble to the surface when people talk about finding a useful equilibrium in their day-to-day life. The common denominator: gentle double duty, coaxing even exfoliation from the follicle level with support and repair of the skin’s moisture barrier.
People often discuss the thoughtful use of specific categories of topical ingredients:
- Gentle Chemical Exfoliants (AHAs & BHAs): Unlike the more gritty, aggressive scrubs, ingredients such as lactic acid or glycolic acid (alpha-hydroxy acids) gently break up the bonds between dead skin cells. Because salicylic acid (a beta-hydroxy acid) is oil-soluble, it may be able to penetrate the follicle and loosen keratin plugs. Those are typically in leave-on lotions or short-contact washes, not full-strength peels.
- Urea: This ingredient is both a gentle humectant (drawing moisture in) and a keratolytic (softening and helping to break down keratin). It’s frequently mentioned for its ability to smooth without harshness.
- Retinoids (OTC): Retinol and other retinoid derivatives may be helpful by normalizing the rate of skin cell turnover within the follicle, which could make plugs less likely to form. There is a need for their painstaking inclusion owing to their irritant nature.
- Moisturize with Ceramides & Lipids is essential to rebuilding the skin barrier. Ceramide, cholesterol, and fatty acid-containing moisturizers assist in restoring the barrier in addition to reducing water loss and the inherent “strength” of the skin.
A critical pattern in successful long-term management is managing expectations and practicing consistency. Changes in skin texture occur over weeks and months, not days. Furthermore, what maintains results is often a simple, consistent maintenance routine, not a complex, aggressive protocol.
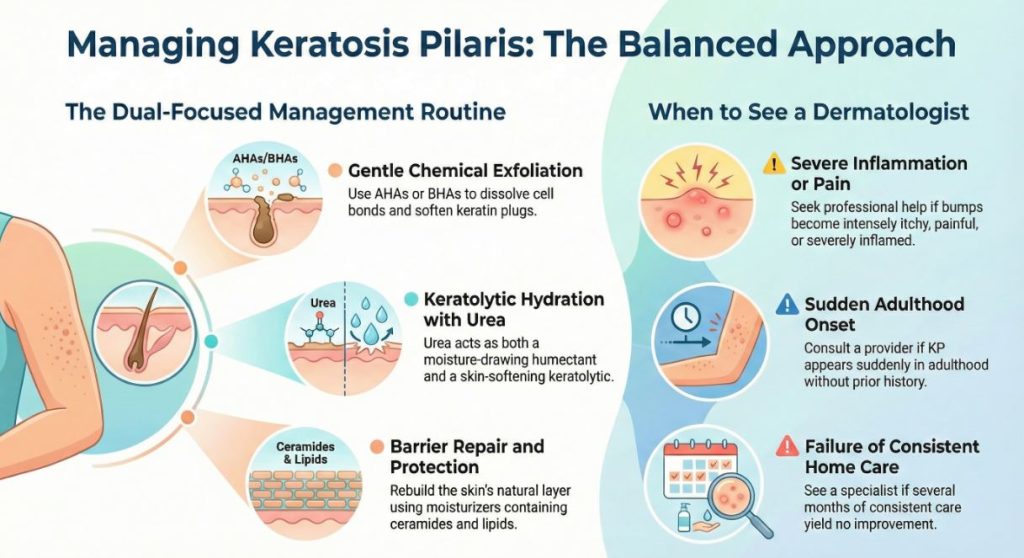
When to Consider a Professional Opinion
While keratosis pilaris is a harmless condition managed through self-care for most, certain signs suggest it’s appropriate to seek guidance from a dermatologist or healthcare provider:
- If the bumps become severely inflamed, painful, or intensely itchy.
- If the condition spreads significantly or appears suddenly in adulthood without a prior history.
- If you are uncertain about the diagnosis, as other conditions can sometimes resemble KP.
- If your carefully managed, consistent home care routine over several months provides no improvement and the appearance significantly affects your wellbeing.
A professional can provide a confirmed diagnosis, rule out other conditions, and may suggest prescription-strength treatment options not available over the counter.
FAQ SECTION
A: For the vast majority of individuals, there is no direct scientific evidence linking specific foods to the cause of keratosis pilaris. It is primarily a genetically influenced skin condition. In rare cases where someone has a suspected underlying condition affecting nutrient absorption, there might be an indirect link, but this is not the norm. The most consistent dietary advice for overall skin health is maintaining adequate hydration and a balanced diet.
A: Because the tendency for KP is written into your skin’s genetic blueprint, complete and permanent elimination is often not a realistic goal for most people. The focus of effective care is typically on management: significantly improving the skin’s texture, reducing the appearance of redness, and minimizing roughness. Many find that with a consistent, gentle routine, KP becomes barely noticeable.
A: This is a fairly widespread misunderstanding. The objective is a light exfoliation beneath the follicle, not to scratch up the surface of the skin. Rough scrubbing can compromise the protective skin barrier, causing more dryness and inflammation, which can cause bumps to appear redder and feel rougher. Milder options, such as using washcloths or chemical exfoliants in leave-on form. They are intended to soften and slough off the keratin plugs without damaging the surrounding skin.
You May Also Ask
A: Absolutely. Genetics decides how likely you are to get a thing; they don’t determine exactly what it looks like. Just as glasses fix genetic sight weaknesses, a good skin care regimen will help keep the genetics that cause KP under control.
A: I know the discoloration (post-inflammatory hyperpigmentation) that can sometimes last after a bump has flattened is typically not permanent. But it can gradually fade over several months. The top way to make them fade is by consistent sun protection, as the sun can darken and therefore slow fading.
A: This might be related to a variety of reasons. Increased humidity in the summer months allows your skin to hold onto more natural moisture. More sun exposure can have a subtle anti-inflammatory benefit, and people wear less clothing, leading to less friction on the arms.
4. CONCLUSION
Getting to know keratosis pilaris starts with recognizing it as a common, harmless variation of skin functioning. Its path to controlling it is not so much a search for a cure as an insistence on consistency and gentleness, respecting the natural biology of your skin.
By concentrating on making keratin plugs softer while not harming the skin barrier, keeping moisture up to it, and trying hard not to lose it, you can whip texture and comfort into shape. The most effective path is informed by patience, realistic expectations, and, when needed, the guidance of a skin care professional.
You may also want to read: Why Thigh Chafing Gets Worse in Summer & How to Manage It
Disclaimer: Disclaimer: This article is a general guide only and is not intended to replace professional medical advice. it is not intended to t.i try o diagnose, treat, cure or prevent any disease or skin condition. Dermatologist always see a doctor or dermatologist for individual recommendations.