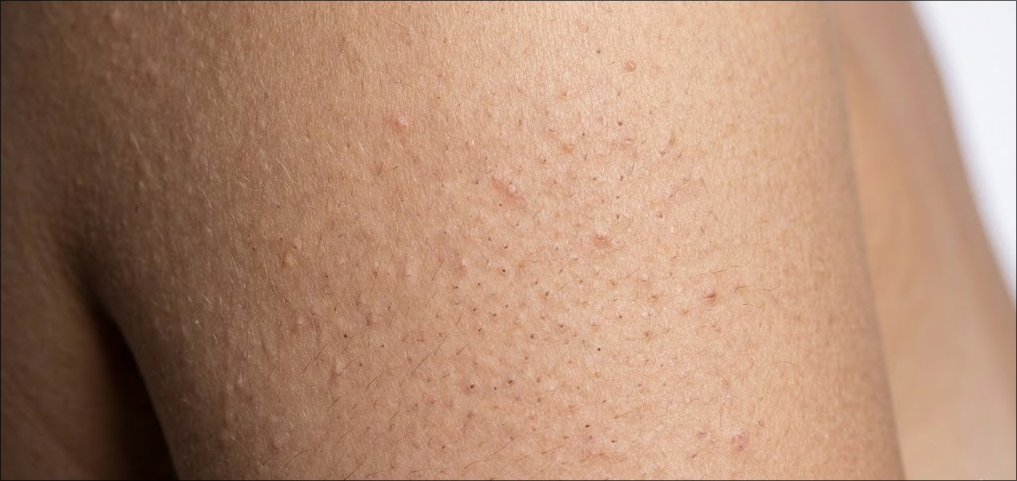
If you notice tiny bumps on your skin that always stays no matter what and never completely vanishes, then these are most likely the classic signs of Keratosis Pilaris (skin condition). Understanding these persistent bumps which are often described as feeling like sandpaper or “chicken skin”—is key to managing this common skin condition.
Dermatologists frequently prefer to view KP as a common skin type rather than a disease, and it’s estimated to affect between 50% and 80% of adolescents and about 40% of adults at some point. This article will help you understand your skin better by explaining what keratosis pilaris is, why it can happens, and the factors that may influence how it appears.
If your skin also feels persistently dry and irritated, see:
Dry Itchy Skin Patches: The Actual Problem and Cure.
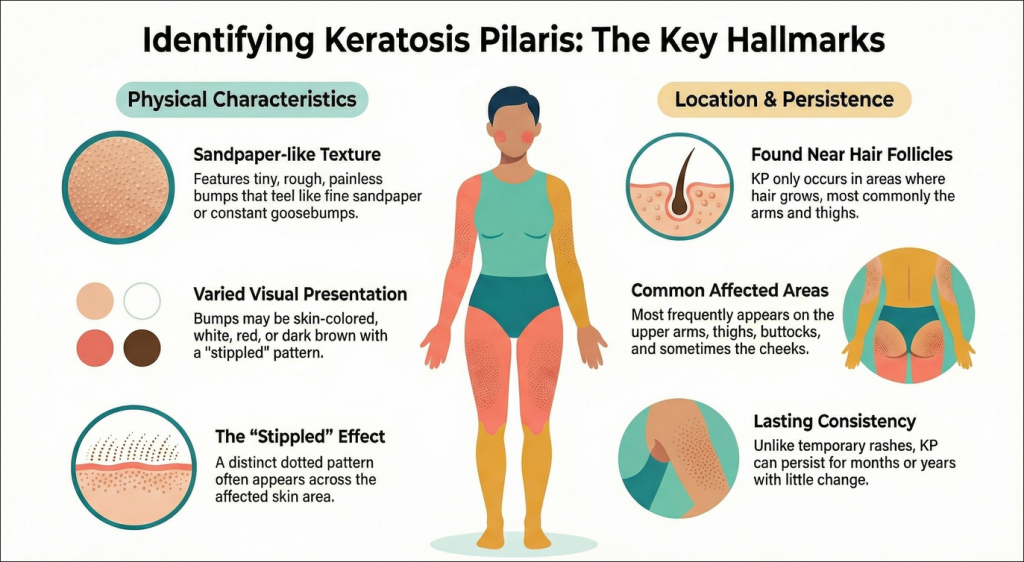
The Hallmarks of Keratosis Pilaris: Recognizing Those Tiny Rough Bumps
The most recognizable thing about KP is that it has an unique texture and appearance:
- Texture and Feel: You will find tiny, rough bumps on the skin that feel like fine sandpaper or something like you are feeling constant goosebumps. The surrounding skin can sometimes feel dry or itchy, these lumps are usually painless and doesn’t harm you anyway.
- Appearance: The bumps are usually same as your skin color. But your skin tone and the level of inflammation can decide wether it looks white, red, or darker brown. You might also see a “stripped” or dotted pattern in the affected area.
- Common Locations: KP most often appears on the upper arms, thighs, buttocks, and sometimes the cheeks. It only occurs in areas where there is hair.
- Persistence: Its consistancy is a key factor that you need to look for. Unlike a rash or pimple that appears and slowly fades away, KP can last for months and even years with no change at all.
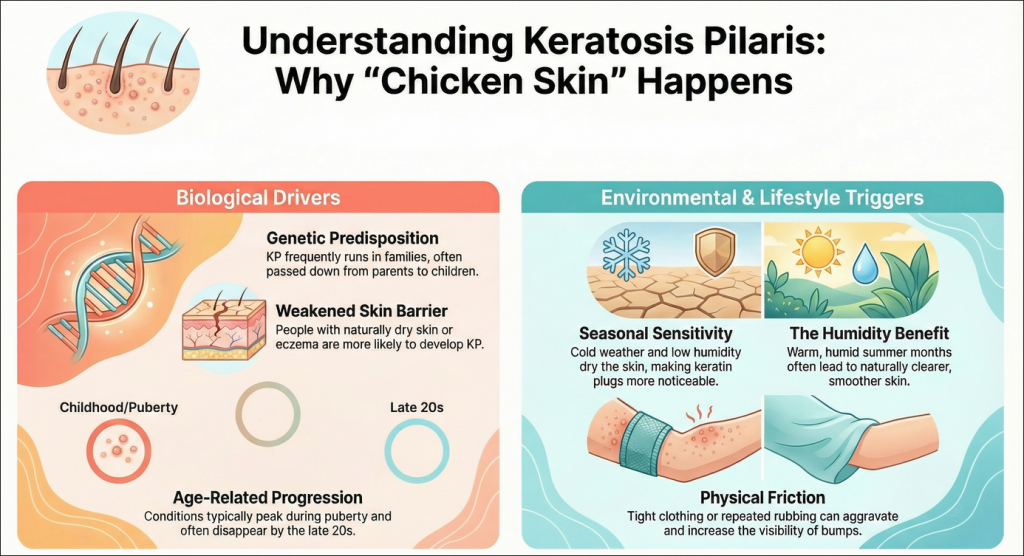
Why It Happens: The Biology Behind Keratosis Pilaris Bumps
Keratosis pilaris is mainly a mild issue with keratin buildup. Keratin, a strong and protective protein, is a key part of your skin, hair, and nails.
People with KP often produce extra keratin for genetic reasons. Rather than naturally shedding, this keratin mixes up with dead skin cells and forms a small, hard plug in a hair follicle. This plug blocks the follicle is the sole reason that traps the hair underneath, which creates the raised bump you see. Sometimes, you might even notice a coiled hair below the bump’s surface.
You cannot catch this condition from someone else. It is harmless and not contagious. It’s simply a variation in how your skin cells turnover.
Contributing Factors and Common Triggers for KP
The primary cause is genetic, but many things can influence how severe KP is and how noticeable it appears:
- Genetics and Family History: KP tends to be hereditary. If a member of your family has it, you are more likely to have it. Skin Conditions:
- Skin Conditions: While anyone can get KP, it’s more common if you already have naturally dry skin or conditions such as eczema because your skin barrier is likely weaker than someone without these conditions. frequently runs in families.
- Age: It occurs most frequently in children and adolescents. It frequently develops in childhood and may also flare up during adolescence, as hormones fluctuate. For most people it gets better or goes away by their late 20s or early 30s.
- Environment and Season: Cold, dry conditions are a high risk factor. The lower humidity also causes the skin to dry out, which in turn makes the keratin plugs and bumpy texture more obvious. For many, KP is less noticeable in the hot, damp summer months.
- Friction: Tight clothing or repeated friction on the skin can aggravate the bumps and make them more visible.
Differentiating Keratosis Pilaris from Other Skin Concerns
People often mistake KP for acne, clogged pores, or other conditions. The table below outlines key differences.
| Characteristic | Keratosis Pilaris | Acne / Clogged Pores | Eczema (Atopic Dermatitis) |
|---|---|---|---|
| Primary Cause | Keratin plug in hair follicle. | Oil (sebum), dead cells, and bacteria clog pores. | Inflammatory condition; skin barrier dysfunction. |
| Common Locations | Upper arms, thighs, buttocks, cheeks. | Face, chest, back, shoulders. | Creases of elbows/knees, face, hands; can be widespread. |
| Texture/Appearance | Tiny, rough, sandpaper-like bumps; skin-colored, red, or brown. | Blackheads, whiteheads, red inflamed pimples, cysts. | Dry, red, inflamed, itchy patches; may scale, crust, or ooze. |
| Typical Sensation | Usually not painful; can be slightly itchy or feel dry. | Can be painful, tender, or itchy. | Intensely itchy, often the main symptom. |
A consistent routine can reduce rough texture over time — learn more:
Morning vs. Night Skincare: What’s the Difference?
Management Approaches for Understanding and Caring for KP
You may have discovered that generic skincare recommendations with KP are ineffective or even detrimental. Here are a few typical reasons:
- Over-Exfoliation Backfires: The urge to remove bumps can exacerbate KP. Without successfully removing the deep keratin plugs, harsh physical scrubs, loofahs, or vigorous brushing can irritate the skin and increase redness and inflammation.
- Focusing on the Wrong Target: Using acne products or oil-stripping cleansers on KP can dry out the skin even more visible with KP because it leaves behind that tell-tale roughness.
- Misunderstanding “Cure”: Curing KP is a genetic, lifelong condition. Texture and appearance are the obsession, rather than a definitive solution. Even treatments that work require regular maintenance, and stopping them often means bumps will return.
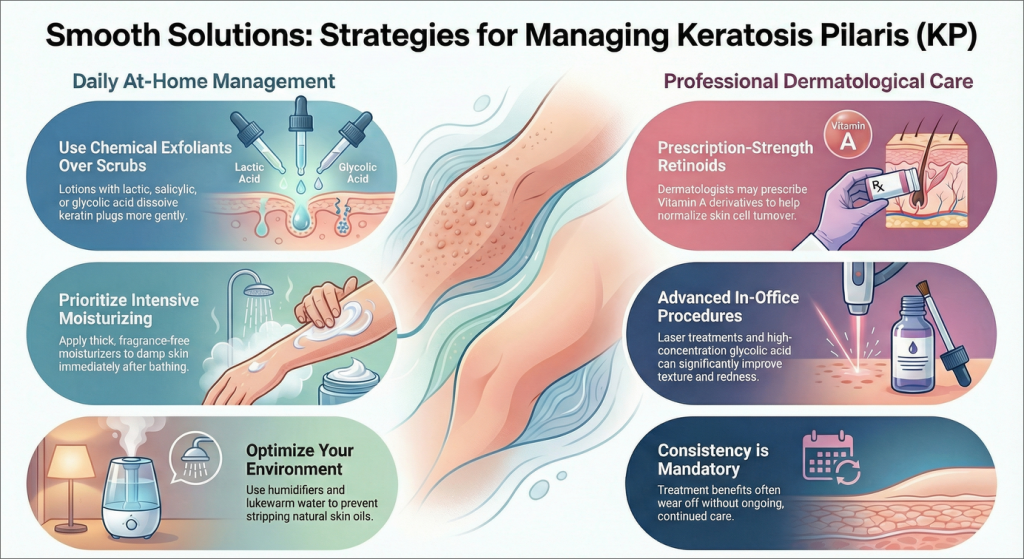
Approaches Focused on Understanding and Management
To deal with KP properly, you need to address dried out skin and normalize the shedding of keratin into your pores allowing the hair to grow as it should.
- Gentle Cleansing and Exfoliation: To exfoliate, a gentle, non-drying skin cleanser. A physical scrub may not be as effective or irritating as a chemical exfoliant (like lotions with lactic acid, salicylic acid, glycolic acid or urea). They work by helping to dissolve and loosen the keratin plug.
- Prioritize Intensive Moisturizing: Thick fragrance-free moisturizer (glycerin, lanolin or hyaluronic acid-based formula) applied to damp skin after a shower traps fluid to decrease dryness and soften the rough texture.
- Environmental Adjustments: The addition of a humidifier in the home can keep skin from drying out, because dry air can trigger KP during winter months. What’s more, opting for lukewarm instead of hot showers also helps to avoid the removal of natural oils from the skin.
- Professional Guidance: If you aren’t seeing the results that you want at home, a dermatologist can offer stronger solutions. These might include cosmetic office procedures such as particular laser treatments, which can improve texture and decrease redness in some people, or prescription-strength retinoids, a family of compounds that are related to vitamin A. For example, while high-concentration glycolic acid based treatments may have a major impact on appearance now, according to her research the affects very well could go away over time if care is not maintained.
When to Consult a Healthcare Professional
Although KP is safe, you should consult a physician or dermatologist if:
- Some people want confirmation, and you are uncertain about the diagnosis.
- The lumps get extremely painful, itchy, or inflamed.
- Your quality of life is impacted or you experience severe distress as a result of the condition.
- You want to talk about other options because you’ve been trying gentle, consistent management for months and you don’t see any improvement.
Frequently Asked Questions
No, they are some what distinct conditions. Acne involves oil glands and inflammation, meanwhile KP is buildup of keratin whithin hair follicles. They can sometimes appear in similar areas (like cheeks) but have different causes and different management approaches.
You can never cure KP permanenly as it is linked to genetic skin function. However, your skincare routine can be a huge factor of consideration to manage it, and it frequently lessens or resolves on its own by late 20s or 30s.
The persistence of KP is mainly because of its genetic nature. Your skin is continuously producing new skin cells and keratin. Without constant management to address the unique way your skin sheds these cells, the plugs can reform. Patience and consistency with care are key, as improvements often can take weeks or months.
In winter the air gets cold and holds less moisture, and indoor heating further dries the air. This suden drop in humidity draws moisture from your skin, leading to increased dryness. Since dry skin exacerbates KP, the bumps and rough texture typically become more pronounced in winter and often improve in more humid summer conditions.
Some research actually suggests a possible link between KP and defficency of vitamin A, but this is not very common for most people. If you suspect a nutritional deficiency, it’s important to discuss it with a healthcare provider rather than trying to fix it on your own.
Yes, KP is more common in children and teenagers than you think. It often first appears in early childhood. Parents should focus on gentle moisturizing and avoid harsh treatments. The condition improves rapidly as the child grows.
Conclusion
Keratosis pilaris is a harmless and common skin feature. Knowing this comes from a genetic predisposition to retain keratin buildup and is heavily related to skin dryness can make you far more equipped to manage your approach with gentle care, rather than frustration. The point isn’t some magical cure, it’s about supporting your skin and treating it kindly; keeping up with the moisturizing, light exfoliation and lifestyle changes.If the appearance of KP affects your wellbeing, seeking professional advice can open doors to a wider range of management options tailored to your skin’s specific needs.
Disclaimer: This article is for educational purposes only and does not replace professional medical advice. Always consult with a healthcare provider or dermatologist for personal medical concerns.