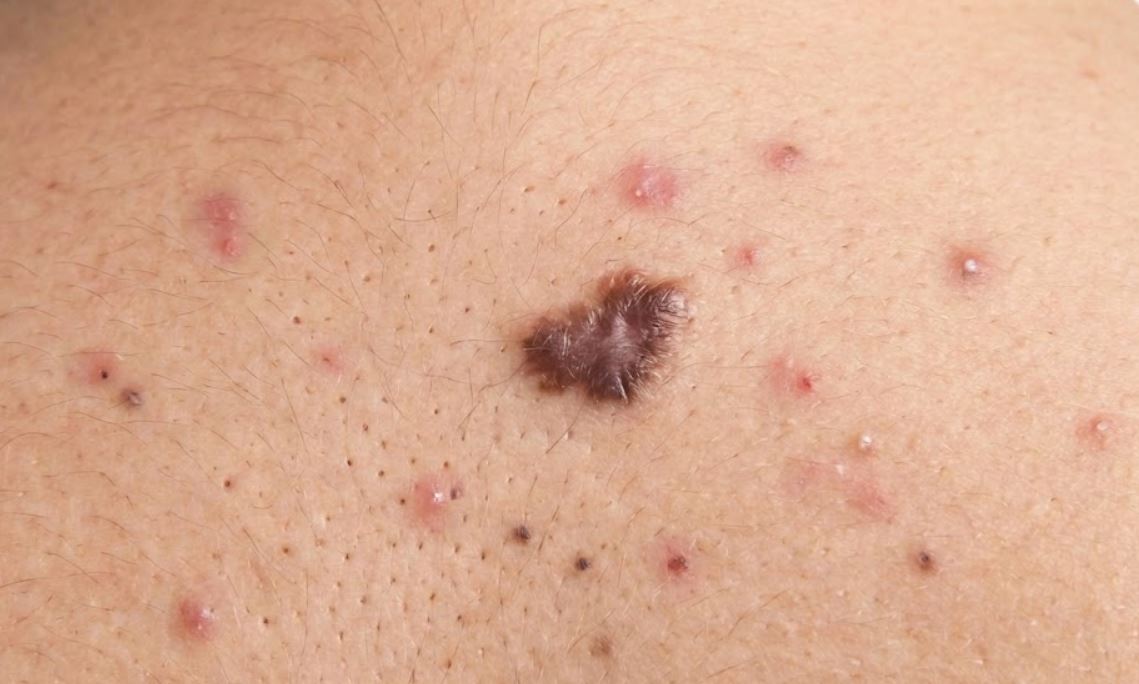
Many people will find that while they may get rid of their active back acne, they’re left with a set of stubborn dark scars known as post-inflammatory hyperpigmentation (PIH) that still won’t seem to disappear long after the pimples have gone. These are flat marks that are pigmented in color (pink, red, purple, brown, or gray-black) but don’t have an indented or textured quality to them.
This article will dig into why you may face the marks on your back, their stubbornness, and how understanding your skin biology and daily habits can form a logical treatment routine.
It’s really just about being able to step back and see the big picture so that you can make your own educated, realistic decisions about what your skin might need. For facial post-acne marks, see: Red Acne Marks That Won’t Fade: A Guide to Stubborn Discoloration.
Why Back Acne Leaves Its Mark: The Biology of Pigmentation
To understand why dark scars linger, we must first look at what happens in the skin during and after an acne breakout.
An acne lesion is a location of intense inflammation. Your inflamed skin causes your skin’s pigment-producing cells, called melanocytes, to become active. This is a natural, though irritating, reaction. The increased melanin can either travel to the surface of the skin or deeper into the dermis, leaving a darker patch that sticks around long after the inflammation has disappeared.
The depth and color they leave on the skin depends to some extent on your skin tone. The residual mark left in lighter skin tones is often erythematous and may appear as red or pink (post-inflammatory erythema) due to some residual dilated blood vessels. In medium to darker skin tones the hyperpigmentation response is more intense, and a brown, gray or deep purple erythema usually results. The deeper value in the dermis is more bluish or greyish and more difficult to treat.
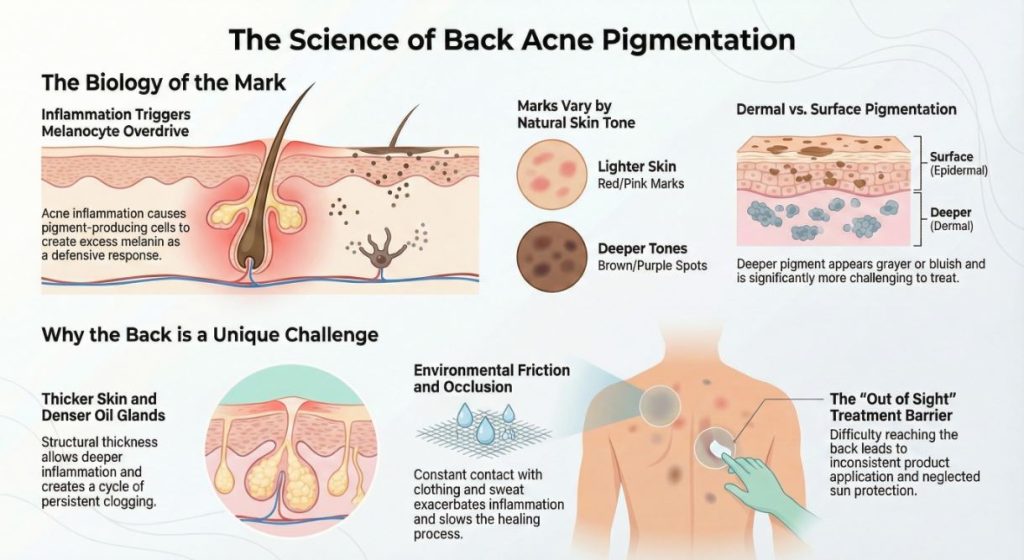
Why the Back Is a Special Challenge
Treating pigmentation on the back isn’t the same as treating it on your face. Several unique factors make “bacne” marks particularly stubborn:
- Thicker Skin & Closer Glands: Thicker Skin & Closer Glands The skin on the back is actually thicker and has more oil glands than delicate facial skin. This means the inflammation can go deeper, and more oiliness can just create a vicious cycle of hard plugs with the chronic pigmentation.
- The ‘Out of Sight, Out of Mind’ Effect: The ‘Out of Sight, Out of Mind’ Effect: In short, it can be difficult to look at and access the back skin, resulting in less frequent use of all products including sun protection (important for pigmented areas to prevent dark marks from worsening).
- Constant Environmental Triggers: Your back is nearly constantly in contact with potential sources of irritation, such as tight clothing, gym clothes, backpack straps, and chair backs, all of which cause friction and occlusion, raising inflammation.
- Why Common Advice Can Feel Confusing or Ineffective
You may have tried popular solutions with disappointing results. This disconnect often stems from advice that doesn’t account for the back’s unique environment.
- The Exfoliation Mistake: Encouraged to have chemical exfoliants (e.g., AHA and BHAs) to accelerate cell renewal, some people take it too far and treat their backs to the equivalent of a face and body scrub, thereby causing micro tears and inflammation, which can then exacerbate pigmentation. Light chemical exfoliant is your friend.
- The Inadequate Sun Protection: Remember when you diligently slapped sunscreen on your face but not your back? Well, the sun’s UV rays are responsible for making hyperpigmentation so persistent. They cause you to produce extra melanin,n which then intensifies the existing imperfections and impedes their removal.
- The Moisturizer Oversight: Many with acne-prone skin avoid body moisturizers, fearing they will clog pores. However, a well-hydrated skin barrier heals more efficiently. Using a lightweight, non-comedogenic (non-pore-clogging) moisturizer can actually support the skin’s recovery process.
- The Friction Factor: Standard advice rarely emphasizes the impact of daily mechanics. Chronic friction and pressure from tight clothes, bags, or even prolonged sitting can create a low-grade inflammatory environment, hindering the skin’s ability to resolve the pigmentation.
If ingrown hairs are leaving marks, read: Ingrown Hair on Bikini Line: Causes, Prevention & Care.
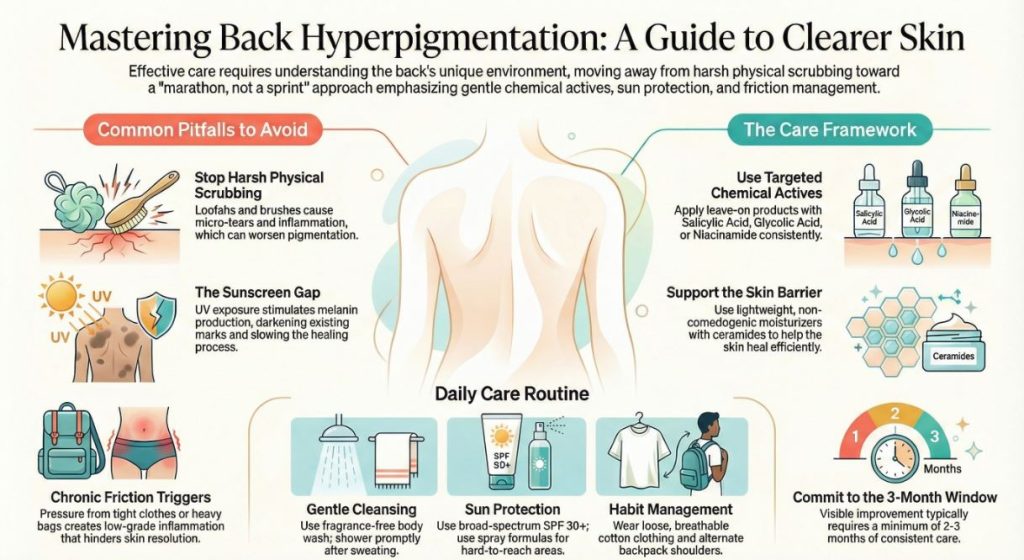
Building a Thoughtful Care Framework
Effective care for back hyperpigmentation is a marathon, not a sprint. It focuses on managing expectations, minimizing new triggers, and patiently supporting the skin’s natural renewal process. The following table outlines a balanced approach that addresses prevention, treatment, and protection.
| Care Pillar | Core Principle | Practical Application for the Back |
|---|---|---|
| 1. Consistent, Gentle Cleansing | Remove sweat, oil, and bacteria without stripping or irritating the skin. | Use a gentle, fragrance-free body wash. After sweating, shower promptly. Avoid harsh scrubbing tools. |
| 2. Targeted Actives | Use ingredients that gently encourage cell turnover and address pigmentation. | Look for leave-on products with ingredients like Salicylic Acid (BHA), Glycolic Acid (AHA), Azelaic Acid, or Niacinamide. Apply consistently, not aggressively. |
| 3. Mandatory Sun Protection | Prevent UV rays from darkening existing marks and causing new damage. | Use a broad-spectrum, water-resistant sunscreen (SPF 30 or higher). Spray formulas or lotion applicators can help reach the back. Reapply after swimming/sweating. |
| 4. Barrier Support | Maintain a healthy skin barrier to optimize healing. | Follow with a lightweight, non-comedogenic moisturizer. Ingredients like ceramides or hyaluronic acid can be beneficial. |
| 5. Habit & Friction Management | Reduce daily inflammatory triggers. | Wear loose, breathable (e.g., cotton) clothing. Change out of sweaty clothes immediately. Alternate backpack shoulders or use a cross-body bag. |
A Note on Application: Consider tools like long-handled lotion applicators or spray formulations to ensure even and consistent product application across the entire back. Patience is essential; visible improvement in back hyperpigmentation typically requires a minimum of 2-3 months of consistent care.
Hormones may also play a role — learn more: Why Does Acne Get Worse Before Your Period?
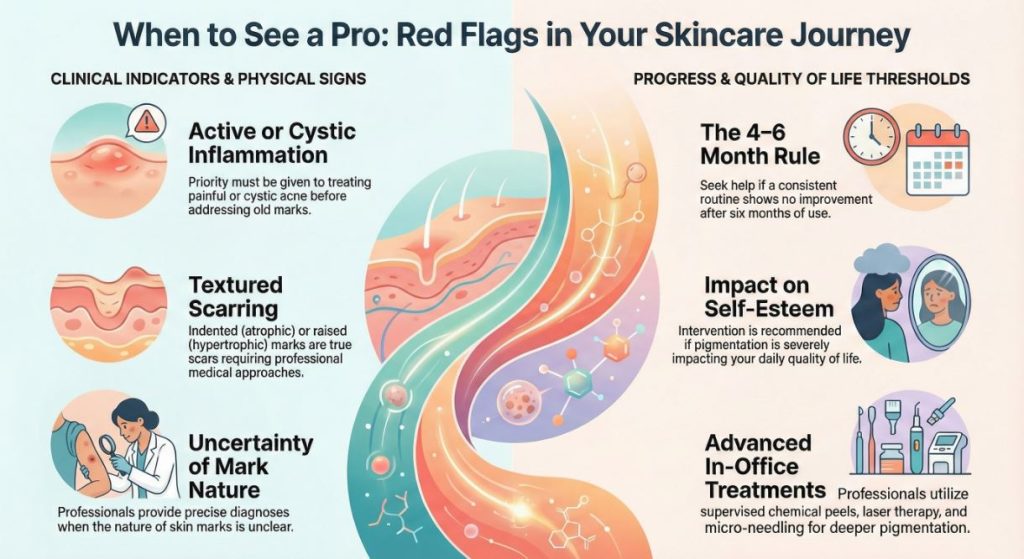
When to Consider Professional Guidance
While a diligent at-home routine forms a strong foundation, there are clear indicators that consulting a dermatologist or licensed skincare professional is a prudent next step. Seeking expert advice is recommended if:
- You are dealing with active, painful, or cystic back acne alongside the old marks, as treating active inflammation is the first priority.
- Your marks are textured—indented (atrophic) or raised (hypertrophic or keloid)—as these are true scars requiring different approaches.
- You have consistently followed a well-structured routine for 4-6 months with minimal to no improvement in the dark marks.
- The pigmentation is severely impacting your quality of life or self-esteem.
- You are unsure about the nature of the marks or need help tailoring a safe and effective plan.
A professional can provide a precise diagnosis, offer in-office treatments like supervised chemical peels, laser therapy, or micro-needling that target deeper pigmentation, and prescribe stronger topical medications if appropriate. They are your partner in navigating this process safely and effectively.
FAQ’S
A dark mark, also known as post-inflammatory hyperpigmentation (PIH) is a flat, discoloured patch on the skin where an acne lesion used to be. A “real” acne scar is a change in the texture – you have those depressions (indented scars) or raised bumps (keloid/hypertrophic scars). While PIH may fade and can be worked on, textured scars usually need true help.
They are not permanent in most cases! PIH is treatable, and it can fade with time, usually requiring a few months to a couple of years. But much of its development relies on sun protection, skin-care practices, and natural skin biology. Uniform care is highly beneficial and helps part with rush.
The skin on your back is thicker and contains more oil glands, making it harder to reach all the time. The result: active ingredients may not penetrate as well, and every day maintenance (like sunscreen) gets overlooked. The First Aid Beauty description is on point – The pimple on my lower back had the texture of a keloid, so inflamed and scarred with brown flakes I was appalled just feeling it while washing in the shower.
You May Also ASk
Without question, apply a broad-spectrum sunscreen (SPF 30+) to your back every single day, and reapply it during prolonged sun exposure.
Still not too late. Older, more established pigmentation may not clear as quickly as fresher pigmentation, but the life cycle of the skin is continuous, and a good routine of gentle exfoliation, inhibiting melanin activity, and persevering with good sun care can make a difference in time.
While diet doesn’t directly “cause” old marks, overall skin health matters. High-sugar diets and significant stress can promote systemic inflammation, which may subtly slow the skin’s healing and renewal processes. The most direct lifestyle factors are sun exposure without protection and wearing irritating, non-breathable fabrics.
Conclusion
There is one final aspect of navigating the unyielding persistence of dark scars caused by old back acne that comes down to patience and diligent, understanding care. These marks are no more indicative of any flaw in you than the many other biological processes that lie at the mercy of the environment—in fact, they are exactly the kind of marks you should expect to see based on your itinerary up to this point.
The best news of all is that the battle against these dark scars can be fought in the time it takes to learn to tolerate delay; it is not a fight that you will win in a matter of days; it is one that spans the course of months, based upon understanding. The evidence will show you that the enemy is a process that can be helped along prudently and politely, by protecting your back diligently from the sun, feeding it sparingly, and embracing the journey on your way to seeing real, lasting improvement.
Disclaimer: This article is for information only and is not intended as a replacement for the professional medical advice, diagnosis or treatment by your dermatologist or any other qualified health care professional. Do not ignore professional advice or delay seeking professional advice because of anything you read here.